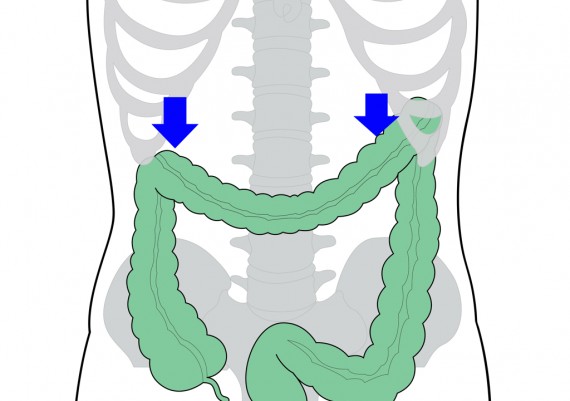
7- 9įrom early cadaveric studies to more recent in-vivo non-physiological experimentation, metastatic routes stretching from the paracolic nodes to the superior mesenteric artery, the MCA, the accessory MCA, the IMA and left colic artery (LCA) nodal basins have been described. 1, 3- 6 However, it is difficult to apply the principles of CME to areas of watershed blood supply such as the splenic flexure (SF) owing to the lack of clarity as to whether SF lymphatic drainage preferences the middle colic artery (MCA) or the inferior mesenteric artery (IMA) nodal basins, or both. This approach has been demonstrated to result in superior specimen quality 1, 2 and convey a survival advantage in several cohort studies. In the era of complete mesocolic excision (CME) and central vascular ligation (CVL), dissection along bloodless embryonic tissue planes with a ‘high’ vascular tie (HVT) theoretically ensures removal of a pre-defined lympho-neuro-vascular package enveloped between intact parietal peritoneum. This may have implications for the surgical approach to SFCs with respect to standardization of CME and CVL surgery for these cancers. However, the survivals of SFCs and non-SFCs are similar, possibly because the most important determinant of outcome, tumour stage, is no different between the groups. SFCs have a distinct phenotype, the individual characteristics of which are associated with poorer survival. No differences were noted between SFCs and non-SFCs with respect to tumour stage ( P = 0.3). These characteristics were associated with poorer survival outcomes. SFCs were more likely to present urgently ( P < 0.001) with obstruction ( P < 0.001) or perforation ( P = 0.03), and more likely to require an open operation ( P < 0.001). SFCs were not associated with OS ( P = 0.6) or DFS ( P = 0.5). Of 2149 patients with colon cancer, 129 (6%) had an SFC. Overall survival (OS) and disease-free survival (DFS) estimates and their associations to clinicopathological variables were investigated with Kaplan–Meier and Cox regression analyses. Clinicopathological data were extracted from a prospective database. MethodsĪn observational cohort study at Concord Hospital, Sydney was conducted with patients who underwent resection for colon adenocarcinoma (1995–2019). This study aimed to compare survival outcomes for SFCs and non-SFCs, and better understand the clinicopathological characteristics which may define a distinct SFC phenotype. The management of splenic flexure cancers (SFCs) in the era of complete mesocolic excision (CME) and central vascular ligation (CVL) is challenging because of its variable lymphatic drainage.
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
